Article Review By Brittany Day
Upper Limb Active Joint Repositioning During a Multijoint Task in Participants with and without Rotator Cuff Tendinopathy and Effect of a Rehabilitation Program
Pairot de Fontenay, Benoit, Mercier, Catherine, Bouyer, Laurent, Savoie, Alexandre, & Roy, Jean-Sébastien. (2019). Upper limb active joint repositioning during a multijoint task in participants with and without rotator cuff tendinopathy and effect of a rehabilitation program. Journal of Hand Therapy, 33(1), 73-79.

The Skinny
This article presents two experiments with two separate study designs related to shoulder proprioception exercises. The first experimental design (E1) is a Level 3 Cross-Sectional study using an assessment on multijoint active joint repositioning in participants with and without RC tendinopathy. This design aims to compare upper limb proprioception abilities of participants with and without RC tendinopathy. The second experimental design (E2) is a Level 3 Prospective Single-Group Pre-Post study to compare proprioceptive skills of participants with RC tendinopathy before and after a standardized six-week treatment protocol.
Errors in active joint repositioning during a multijoint task increased in patients with rotator cuff (RC) tendinopathies compared to controls indicating proprioceptive challenges that affect the upper extremity. Following a standardized protocol for RC tendinopathy for six weeks may improve functional limitations, RC tendinopathy symptoms, and active joint repositioning previously experienced by the patient. These findings may result in a quicker return to normal daily activities for the individuals involved.
In The Weeds
RC tendinopathy participants recruited via electronic mailing list provided by a local university and private medical/physiotherapy clinics. Participants were approached if they met the inclusion criteria in at least one positive sign in the following three categories: (1) pain during flexion and abduction, (2) positive Neer’s or Kennedy-Hawkins tests, and (3) pain on resisted isometric external rotation (ER) and abduction or empty can test. Participants were excluded if they met any previous shoulder surgery, shoulder pain reproduced by neck movement, or clinical signs of full-thickness RC tears/shoulder capsulitis. Healthy participants were recruited in the local community. The article reports 63 total participants; (1) RC tendinopathy for E1 N=20, (2) healthy control group N=20, and (3) Participants with RC tendinopathy for E2 N=23.
E1 compared active joint repositioning abilities during a multijoint task. The assessment used was a 0.7 x 1.20-meter flat surface covered by plexiglass paneling. The blindfolded participants’ hand is attached to a hand cone with wheels that supports a laser pointer. This could project the hand position onto the plexiglass without providing visual cues to the participant. The standardized starting position for each participant was 0 degrees shoulder flexion, neutral rotation, and elbow at 90 degrees. Each participant was passively moved through 12 trials, including 4 in shoulder ER, 4 in shoulder internal rotation (IR), and 4 in shoulder neutral rotation (NR). The participants’ hands were placed at each location for 5 seconds before returning to the starting position and actively moving their upper extremity back to the same area. The difference between the active and passive regions was measured in millimeters. The percentage of global mean error was calculated between the two groups.
E2 intervention included a standardized six-week RC tendinopathy described in a recent study by Fourneir-Belley et al which provides for movement training, manual therapy, strengthening, stretching exercises, and patient education. Pre and post-testing included the Disability of the Arm Shoulder and Hand (DASH) questionnaire and active joint repositioning assessment (outlined above). Participants and examiners were blinded to group attribution.
Bringing it Home
The results showed a statistically significant difference between the RC group and control with the RC group experiencing more errors in active joint repositioning. Further research is required to determine whether deficits in proprioception are associated with symptoms/functional limitations.
E2 determined self-reported symptoms, functional limitations, and active joint repositioning deficits significantly improved following a standardized 6-week protocol for RC injury. After a 6-week intervention, participants with deficits in active joint repositioning at baseline significantly improved their ability, while participants without deficits remained the same. It should also be noted there was no significant difference in DASH scores between the participants who had active joint repositioning deficits versus those that did not; however, all showed improvement. Global mean error was used to determine the effect of active joint repositioning error. Paired t-tests were performed to determine the effect in DASH scores and active repositioning error.

Limitations of E1 include the differences in age; however, a regressing analysis showed no significant age-related differences between the two groups in terms of active joint repositioning errors. E2 limitations include a lack of control group and randomized control clinical trial, making this design a lower level of evidence.
More To Read
Hand Therapy Marketing 101
Marketing 101 – 5 Tips for Your Therapy Clinic Confession: I hate marketing. It’s my least favorite part of my job. It is so hard to open yourself up to that much rejection but still stay positive. It feels like the professional version of blind dating, except the other person probably already has a significant…
Read MoreHandlebar Palsy also known as Ulnar Nerve Compression
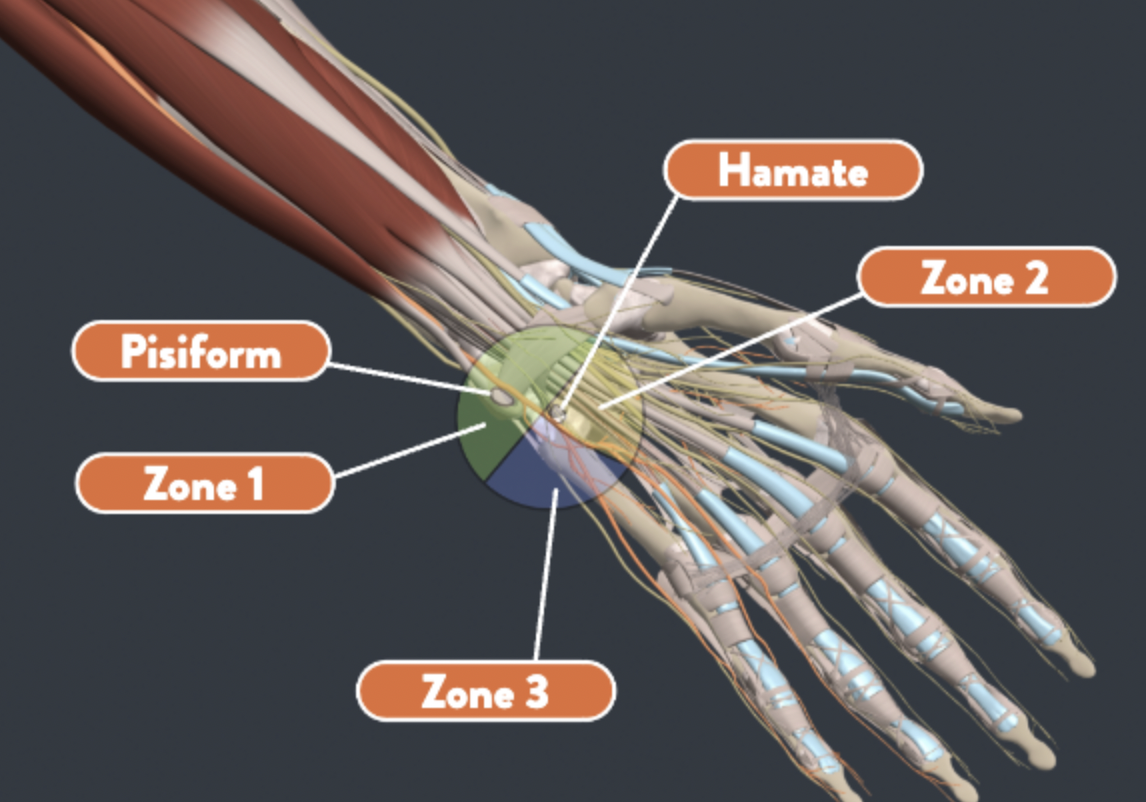
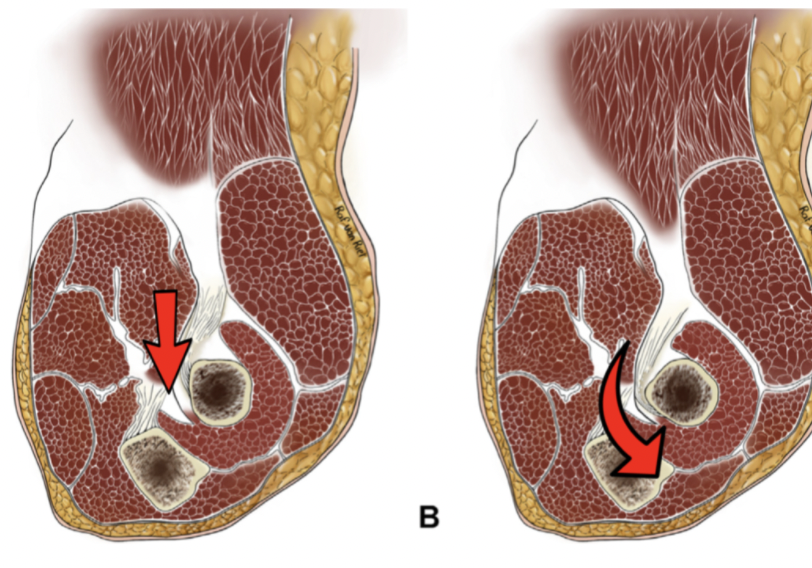
Handlebar Palsy also known as Ulnar Nerve Compression Handlebar palsy, also known as ulnar nerve compression, is a condition commonly experienced by cyclists due to prolonged pressure on the ulnar nerve at the wrist in an area called Guyon’s Canal. This pressure can occur from putting pressure on the handlebars or gripping the handlebars tightly. …
Read MoreNew Distal Bicep Tendinopathy Provocative Test for Hand Therapist
Caekebeke, P., Schenkels, E., Bell, S. N., & van Riet, R. (2021). Distal biceps provocation test. The Journal of Hand Surgery. The Skinny: These surgeons were looking for a provocative test for distal bicep tendinopathy (distal biceps tendonitis test), specifically partial tears, that was more sensitive and specific. Complete tears are more easily tested in…
Read MoreSign-up to Get Updates Straight to Your Inbox!
Sign up with us and we will send you regular blog posts on everything hand therapy, notices every time we upload new videos and tutorials, along with handout, protocols, and other useful information.