By: Amalia Garcia
Introduction
After completing three weeks of my Level II hand therapy rotation, I have seen a wide variety of common upper extremity injuries such as carpal tunnel syndrome, distal radius fractures, mallet finger, flexor tendon lacerations, arthritis, and more. One condition that stood out to me was one that I hadn’t heard of before that is not commonly seen in this setting. I saw a patient who had recently undergone surgery to remove his flexor digitorum superficialis (FDS) that had been damaged by a rare blood condition called Arteriovenous Malformation (arteriovenous malformation hand). Since I had never heard of this specific condition, I decided to do a little research and learn more about the patient’s medical history through his operative report, initial OT evaluation, and past daily notes so I could get a better understanding of the progress he has made over the past four weeks since the procedure.
What is Arteriovenous Malformation?
Arteriovenous malformation (AVM hand) is a rare congenital vascular disorder that causes tangles and atypical connections between arteries and veins (Kim et al., 2021). These tangles, or malformations, cause the blood to bypass the capillaries and disrupt the normal blood flow circulation to the area of the body where it is located. Typically, AVM’s occur in the brain and spine but can occur anywhere in the body, like in this patient’s case, in his left forearm. When an AVM occurs peripherally, it can cut off blood flow to surrounding tissues and cause damage. Some individuals with AVM may never present with noticeable signs and symptoms, while others with peripheral AVM may present with pain to the affected area, muscle weakness, edema, visible lumps in the affected area, and sores and ulcers on the skin.
AVM and Hand Therapy
The patient presented to therapy the day after AVM hand surgery with his mom, who assisted with providing the patient’s medical history. She stated that when he was five, she noticed his left arm felt “squishy” like there was a lot of fluid in it. After two years of testing, he was diagnosed with AVM of the forearm (AVM in hand). Over time, the AVM hardened, and the patient developed a Volkmann’s wrist contracture, keeping him in 90 degrees of wrist flexion. The patient then underwent surgery to remove the AVM, FDS, flexor carpi radialis tendon release, palmaris longus tendon lease, carpal tunnel release, cubital tunnel release, and median and ulnar nerve neurolysis. This means that the AVM primarily affected these structures, but the FDS was the primary muscle that was damaged and needed to be removed. The other muscle tendons were released due to the contracture formation. The contracture and the AVM itself compromised the median and ulnar nerves, which resulted in the carpal tunnel and cubital tunnel release and neurolysis of the nerves from the AVM.
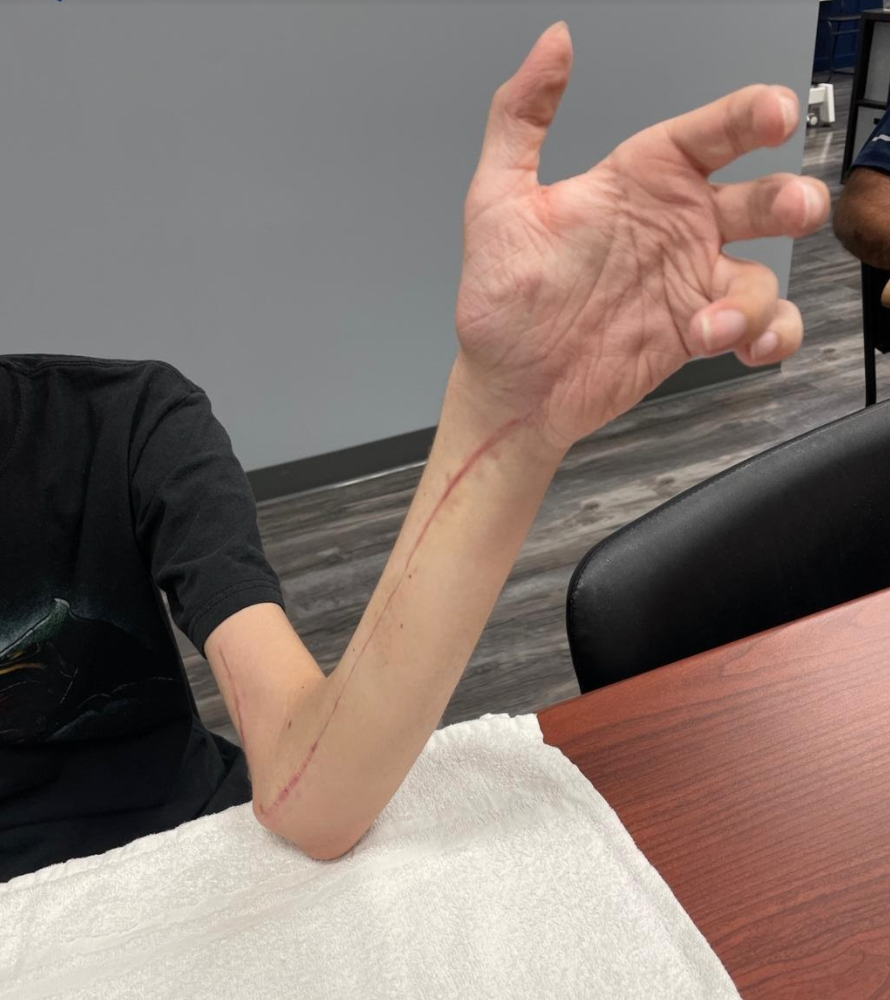
The patient presented to the evaluation with an incision line from the palm to the medial elbow. The therapy orders included AROM/PROM of the wrist, thumb, and digits, suture removal, and an order for a custom orthosis. His limitations included pain (5/10 at worst), limited ROM in the elbow, wrist, and digits, and decreased strength. The therapist fabricated a custom resting hand orthosis to keep the wrist neutral and the digits in extension.
What’s the Goal?
For this specific patient, his main goal is to return to playing baseball in the Fall. In addition, he relies on his right upper extremity to perform all ADL and IADL tasks and guards his left upper extremity after the procedure.
To reach the patient’s chosen goal, the first step in therapy is to work on the ROM of his left shoulder, elbow, wrist, and digits to avoid stiffness and promote mobility. It is also important to address the surgical scar early on through scar mobilization and massage to minimize fascial adhesions and promote tendon gliding. Lastly, it is important to increase his functional gross grasp and pinch strength needed to use his left upper extremity for daily functional tasks.
Conclusion
AVM is a rare condition to occur in the upper extremity. It is important to take the time to research any diagnoses that a patient may have to implement better an effective treatment plan to help patients get back to being functional and independent in their valued occupations.
References:
ACR, R. S. N. A. and. (2020, January 21). Arteriovenous Malformations (AVMs). Radiologyinfo.org. https://www.radiologyinfo.org/en/info/avm.
Kim, R., Do, Y. S., & Park, K. B. (2021). How to Treat Peripheral Arteriovenous Malformations. Korean Journal of Radiology, 22(4), 568.
Mayo Foundation for Medical Education and Research. (2021, January 1). Arteriovenous malformation. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/arteriovenous-malformation/symptoms-causes/syc-20350544.
U.S. Department of Health and Human Services. (n.d.). Arteriovenous Malformation Information Page. National Institute of Neurological Disorders and Stroke. https://www.ninds.nih.gov/Disorders/All-Disorders/Arteriovenous-Malformation-Information-Page
.
3 Comments
Leave a Comment
More To Read
Hand Therapy: Does Dry Needling work to Treat Trigger Finger
By: Taylor Volentine Reference: Azizian, M., Bagheri, H., Olyaei, G., Shadmeher, A., Okhovatpour, M. A., Dehghan, P., Jalaei, S., Sarafraz, H. (2019). Effects of dry needling on tendon-pulley architecture, pain and hand function in patients with trigger finger: a randomized controlled trial study. The Journal of Physical Therapy Science, 31. 295-298. doi:10.1589/jpts.31.295 Photo retrieved from…
Read MoreTrigger Finger… Quick and Dirty!
This is for you… Hand Therapists! Stenosing tenosynovitis, otherwise known as trigger finger, is a common condition affecting children and adults of all ages. Fast Facts Trigger finger usually occurs at the A1 pulley It occurs with inflammation of the tendons and sheaths of fds and fdp The digit can lock in both flexion and…
Read MoreWound Healing in Hand Therapy
By: Maddie Mott Wound healing (healing hand therapy) involves a complex series of interactions between different cell types, cytokine mediators, and the extracellular matrix with its four basic stages including hemostasis, inflammation, proliferation, and remodeling (Mackay & Miller, 2003). Because successful wound healing requires adequate blood and nutrients to be supplied to the site of…
Read MoreSign-up to Get Updates Straight to Your Inbox!
Sign up with us and we will send you regular blog posts on everything hand therapy, notices every time we upload new videos and tutorials, along with handout, protocols, and other useful information.





Interesting
What was the outcome? Is the kiddo still in treatment?
Baseball would be tough to get back into after this…
My daughters name is Amalia!!
Amalia, Hopefully you can share how the patient progresses with therapy. Thank you for sharing .
I AM 63 YEARS OLD & HAVE AN AVM IN MY RIGHT FOREARM. I HAVE HAD 3 EMBOLIZATIONS. THE LAST ONE THE RADIOLOGIST MISTAKENLY EMBOLIZED AN ARTERY INSTEAD OF THE VEIN. I WOKE UP DURING THE PROCEDURE, IT WAS SO PAINFUL. THE FLESH IN THAT AREA STARTED TO NECROSE (DIE) IT BEHAVED LIKE A BURN THE FLESH DIED FROM THE INSIDE OUT & I NOW HAVE A HUG SCAR ON MY UPPER ARM JUST ABOVE MY ELBOW. I AM NOW HAVING AN ISSUE WHERE WHEN I ROTATE MY ARM THERE IS INCREDIBLE PAIN. MY FAMILY PHYSICIAN TOOK AN XRAY & I HAVE A FRACTURE IN THE ULNA WITH A SMALL PIECE OF BONE STICKING OUT. I AM USING VOLTAREN GEL FOR PAIN & INFLAMMATION & IT IS HELPING. IS IT COMMON TO HAVE FRACTURES IN THE ARM BECAUSE OF THE AVM AS WE AGE? IS THERE SOMETHING I CAN DO TO PREVENT THIS. I HAVE NOT FALLEN OR ANYTHING. A LONG TIME AGO, WHEN I HAD IT XRAYED, THE ORTHOPEDIC DR. SAID MY BONE EDGES LOOKED LIKE MOTH EATEN PAGES.